Contact: Steven Lee, 210-450-3823, lees22@uthscsa.edu
A day after baby CJ’s heart stopped, twice, his parents were presented grim options including a future for him hooked to machines or in end-of-life hospice care.
Something kept them going, a feeling that they were better prepared than most for months of continuing treatment and life-and-death decisions. CJ was delivered prematurely with cyst-filled kidneys three times larger than normal for a newborn. They would grow bigger than adult kidneys, even, and pressure his lungs and heart.
Ultimately, both kidneys were removed, and CJ received a new one – from his mom … a kidney doctor. His dad is a critical-care lung doctor. Both parents discovered, weeks after CJ’s birth, they were carriers of a deadly form of polycystic kidney disease, or PKD, their baby contracted.
Along the way, CJ’s cause became one of the nation’s largest fundraisers for PKD research, with a new effort soon. But the gift he has given his parents is that of a growing toddler now approaching his second birthday and saying his first words: “momma” and “dadda.” And more: a fresh, role-reversing perspective for treating their own kidney and lung patients.
“It certainly makes me approach patients very differently … how I explain things to them and how I relate to them,” said mom, Ashley Garcia-Everett, MD, an adult-kidney physician at The University of Texas Health Science Center at San Antonio, also known as UT Health San Antonio. Her husband, Dr. Christopher Everett, is in private practice at a local hospital.
Of the couple’s story, UT Health San Antonio’s nephrology, or kidney, division chief Kumar Sharma, MD, said: “It is heroic – as both of them worked tirelessly to closely support their son, not only as parents but as highly trained professionals.”
Hour to hour
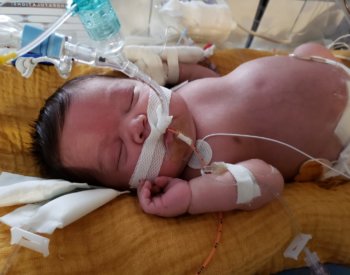 The first sign of trouble came about a month before CJ was born. Dr. Garcia-Everett was hospitalized when it was discovered that the amniotic fluid surrounding the fetus, providing protection and nutrients, was low. Also, sonograms showed slightly enlarged kidneys in the developing baby.
The first sign of trouble came about a month before CJ was born. Dr. Garcia-Everett was hospitalized when it was discovered that the amniotic fluid surrounding the fetus, providing protection and nutrients, was low. Also, sonograms showed slightly enlarged kidneys in the developing baby.
CJ, short for Christopher Javier, after his dad, was born six weeks premature at about 5 pounds in September 2019, at University Hospital in San Antonio. He had a weak cry, pointing to lung problems, so in his first few hours, he was intubated and quickly put on a ventilator – a breathing machine, essentially life-support.
He also wasn’t urinating, so by the fourth day, he was on dialysis, a treatment that helps do the kidneys’ job of filtering blood of unwanted toxins, waste and excess fluids. Doctors knew to expect lung issues, as there is a link between that and low amniotic fluid. What they didn’t know, exactly, was why his kidneys weren’t working well. So, they did genetic testing to see if there was an inherited link, although results wouldn’t be known for several weeks.
The couple had lost their first child during pregnancy because of kidney disease. The dad knew that a typically adult form of PKD ran in his family – autosomal dominant polycystic kidney disease, or ADPKD. The parents didn’t imagine that both of them were carriers of autosomal recessive polycystic kidney disease, or ARPKD, a rare and severe childhood form. That was CJ’s dire diagnosis.
“Approximately one in three newborns with ARPKD dies within the first week of life,” said Mazen Arar, MD, division chief of pediatric nephrology at UT Health San Antonio, and CJ’s kidney doctor. “Both parents were faced with critical decisions daily – if not a few times a day.”
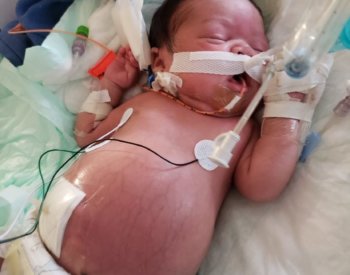 The ventilator would come off, go back on, come off. CJ continued peritoneal dialysis, which uses the lining of the belly to filter the blood, with fluids exchanged through a surgically inserted catheter.
The ventilator would come off, go back on, come off. CJ continued peritoneal dialysis, which uses the lining of the belly to filter the blood, with fluids exchanged through a surgically inserted catheter.
After a while, CJ improved and was taken off dialysis. But with the catheter still in, he developed an infection. On top of that, his kidneys kept growing, putting more stress on his lungs and heart.
CJ had trouble breathing again, so back came the ventilator. He developed high blood pressure, common for kids with kidney disease. He’d have scary spells in which oxygen levels would drop and he’d turn blue, even while on the breathing machine.
One day, his oxygen got so low that his heart rate dropped, too. He “coded” twice that day – his heart stopping and needing revival with CPR. Then came the sober sit-down with a doctor specializing in the care of newborns, laying out options that would determine the course of CJ’s young life.
“That (kind of) conversation that my husband and I have had with so many other patients was such a role reversal,” Dr. Garcia-Everett said, “because we were being sat down to have that conversation of, ‘Should we continue aggressive measures, or should we think of palliative or hospice care for him? Could he make it, and if he made it, what would that look like? Would it be a good quality of life for him or not?’
“There was a lot of concern that as sick as he was, that he might not make it,” she said. “We were incredibly emotional at the time. We really didn’t know what was going to happen hour to hour. They wanted us to have all the options.”
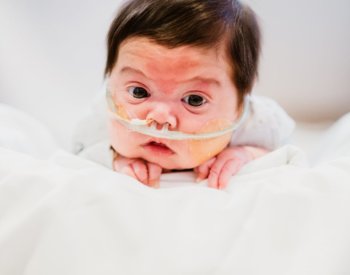 Palliative care and hospice essentially mean relieving the symptoms. But the parents feared CJ could end up permanently hooked to a ventilator and on continual dialysis. Perhaps a breathing tube would need to be inserted by tracheostomy, through a hole at the front of his neck and into his windpipe. He also faced possible neurological damage from being deprived of oxygen when he’d coded.
Palliative care and hospice essentially mean relieving the symptoms. But the parents feared CJ could end up permanently hooked to a ventilator and on continual dialysis. Perhaps a breathing tube would need to be inserted by tracheostomy, through a hole at the front of his neck and into his windpipe. He also faced possible neurological damage from being deprived of oxygen when he’d coded.
At the same time, “We didn’t want to just keep doing things to him to keep doing things to him, without him having a good or reasonable quality of life,” mom said.
Finally, she said, “Our feeling was that if anybody could be prepared to deal with as medically complicated a baby, it was us. As long as he still had a reasonable chance … as long as we could see he could make it out of this and there’s some path we could follow, that was what kept us going.”
A hard stop
Even so, they set a limit on how long they’d agree to treating CJ with his kidneys still in, before having either or both removed.
After the coding scare, doctors got CJ’s blood pressure under control and eased him off the ventilator. With him still unstable, nobody believed that taking out a kidney was a good idea just yet.
But the parents found no clear medical consensus on when the right time would be, even after considerable research – some done on cell or laptop while sitting at CJ’s bedside, consulting with experts worldwide. “That just speaks to how rare this condition is,” his dad said.
So, they held off, but decided on a “hard stop”: If CJ had to go back on the ventilator, they’d do it.
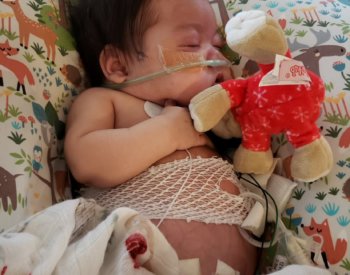 “Many of these decisions were extremely difficult, especially absent consensus,” Dr. Arar said. “Every decision has its consequences. What if the kidneys are removed and CJ develops a major surgical complication? What if they delay the removal of the kidneys and the kidneys lose their remaining little function, leading to CJ needing dialysis anyway?”
“Many of these decisions were extremely difficult, especially absent consensus,” Dr. Arar said. “Every decision has its consequences. What if the kidneys are removed and CJ develops a major surgical complication? What if they delay the removal of the kidneys and the kidneys lose their remaining little function, leading to CJ needing dialysis anyway?”
CJ did OK for several weeks, but then grew more uncomfortable. Sonograms showed the kidneys getting still larger, and he started having trouble breathing … again. Back on the ventilator.
That triggered an initial plan to remove one kidney, and leave the other one in, if possible. Leading up to the surgery at University Hospital, however, CJ’s condition quickly became so critical that doctors didn’t know whether they could even do that much.
CJ’s dad, who tends to critically ill lung patients at Methodist Hospital Northeast in San Antonio, as part of the private-practice group Texas IPS, kept vigil the night before, staying up with his son and watching his vital signs. “It was terrifying,” he said. “Just knowing what I know, and seeing how sick he was getting, I was thinking unless something miraculous happens, he’s probably going to die in the next day or two. It was probably one of the darkest nights of my life.”
By morning, doctors weren’t sure the baby could survive anesthesia. The parents felt defeated, fearing they’d waited too long and let CJ down. They believed if the operating room didn’t take him then, he wasn’t going to live.
“And his surgeon agreed,” mom said. “He said he’s on the precipice. This is our chance. And if it’s going to make a difference, it will make a difference now. There didn’t seem to be much more we could do for him.”
The surgeon, Dr. Barry Cofer of San Antonio Pediatric Surgery Associates, successfully removed the kidney, and that instantly reduced the support needed from the ventilator. The organ had grown to a cyst-bulging 15 centimeters long, compared with 10-12 centimeters for an adult.
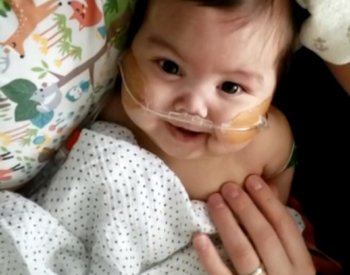 But CJ’s remaining diseased kidney kept growing and needed to be removed just more than a week after the first – this one measuring 17 centimeters. Two days later, he was able to come off the ventilator, but now with no kidneys, he needed daily peritoneal dialysis and support keeping his lungs open.
But CJ’s remaining diseased kidney kept growing and needed to be removed just more than a week after the first – this one measuring 17 centimeters. Two days later, he was able to come off the ventilator, but now with no kidneys, he needed daily peritoneal dialysis and support keeping his lungs open.
Even with all the hookups, the team made it possible for CJ’s parents to hold him. “And when we held him, we held him for a really long time,” mom said. “We would hold him for hours … as long as we possibly could. Even if he was sedated and not always awake, he would still squeeze your finger, which was amazing.”
After six long months in the hospital, CJ and his parents could come home – just in time for COVID-19.
Not going back
What otherwise might have been a well-planned sendoff from the hospital became a rush to get out, ahead of the pandemic that took serious hold in March 2020. Avoiding infection for a very fragile CJ became a priority.
 “Honestly, we were worried 24 hours a day for the first couple of months,” mom said, “because any small thing could set us back to being in that place again.”
“Honestly, we were worried 24 hours a day for the first couple of months,” mom said, “because any small thing could set us back to being in that place again.”
Meanwhile, dad was having to see and intubate COVID-19 patients at his work, as a lung ICU doctor. “There was a lot of anxiety,” he said. “Is dad going to bring COVID home and get mom and baby sick?”
Beyond that, CJ needed to grow and develop, to meet minimum requirements for a kidney transplant. He weighed only about 15 pounds, needing to gain more than half that much by his first birthday, and improve his nutrition and heart function.
When he got home, he couldn’t sit up on his own or easily lift his arms. Almost all his abdominal muscles had been cut at some point, with large incisions from either side of his back and around to nearly his entire stomach area. He needed to be fed through a tube in his belly. Dialysis continued.
 Because he had been on a ventilator, his lungs were weak, too. He would cry without making a sound.
Because he had been on a ventilator, his lungs were weak, too. He would cry without making a sound.
Slowly, though, he gained strength, and his cry went from silent to a scream. Aside from hitting his medical milestones, CJ also worked on just being a “happy, silly baby,” his mom said, with toys and playing peekaboo with things around him.
Importantly, he was able to avoid a return to the hospital – until close to transplant time.
Lifting a fog
Dr. Garcia-Everett knew she was favored to provide a kidney to CJ. Living-kidney transplants are better, she says, as live organs last longer – important for children transplant recipients, as they’ll still need another kidney later in life. And, as she shares 50% of CJ’s genetics, a good match is more likely.
 For others to be considered, there would be an extended process, meaning more time on dialysis for CJ. And her kidney might be small enough; as she says, she’s “not a tall person.”
For others to be considered, there would be an extended process, meaning more time on dialysis for CJ. And her kidney might be small enough; as she says, she’s “not a tall person.”
But all this produced another role-reversing talking-to. Only, it was to herself.
“As a kidney doctor, it was terrifying to think … ‘OK, I know I’m only going to have one kidney’ … and I counsel (patients), ‘You only need one kidney, you only need one kidney … that one kidney can grow and make up for the other one,’ ” she said. “And so theoretically, I knew this. But accepting that for myself, even if it was my son and I absolutely wanted to do it, definitely was scary from the perspective of having him and me go through surgery at the same time.”
CJ’s transplant was scheduled for December, at University Hospital. There were more ups and downs. He developed an infection, delaying the transplant a month. Then, another fever. The parents wondered whether it ever was going to happen, or if it should wait. But the surgical team wanted to push through, and the new date was set for Jan. 28.
Admittedly, said dad, sending both his wife and son off to surgery that morning “was kind of a moment of vulnerability, a moment of surrender, a moment of just letting go and saying the decision is made and we’re going to do this. We had a lot of people praying for him and mom.”
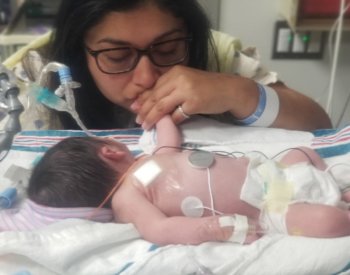 The transplant by Gregory Abrahamian, MD, a surgeon of the UT Health San Antonio Transplant Center, was challenging, and delicate. “I still don’t know how he did what he did,” dad said. “There is not a lot of space in CJ’s belly to put her kidney into him. But it went great, and he and the surgical transplant team did an amazing job.”
The transplant by Gregory Abrahamian, MD, a surgeon of the UT Health San Antonio Transplant Center, was challenging, and delicate. “I still don’t know how he did what he did,” dad said. “There is not a lot of space in CJ’s belly to put her kidney into him. But it went great, and he and the surgical transplant team did an amazing job.”
Since then, CJ’s mom says, he’s become a “totally new baby.” He smiles and laughs more. His energy level is higher. While he still is fed through a tube, he tolerates it better, while taking small samplings of food by mouth. He sits up completely on his own – and can flip over on his stomach and pull himself up to stand. He’s trying to walk, but has taught himself to bear-crawl in the meantime.
More muscular now, he has gained weight, approaching 30 pounds, with better endurance. He’s forming his first words, and learning baby sign language.
Milestones he wasn’t meeting before, he’s blasting past now. “It was like a fog was lifted with him,” she said.
Another milestone: Last year, CJ was recognized as one of the nation’s biggest individual fundraisers for the Walk for PKD, of the PKD Foundation – funds for awareness and research. An online page created in his name brought in $8,127, topping a goal of $7,000, mostly from supportive family and friends, and his mom’s colleagues in the UT Health San Antonio nephrology division.
His effort was part of the division’s team that raised a total of $10,515 – a good chunk of a total $80,000-plus brought in for the San Antonio Walk for PKD 2020. Fundraising for the 2021 event this fall is gearing up.
There is no cure for PKD, yet. It is an inherited disease, with only rare cases of it developing spontaneously. That is why genetic testing is becoming more available.
 Generally, there are treatments to control symptoms or complications, help slow the growth of cysts, and help prevent or slow the loss of kidney function. Those include medication and lowering blood pressure, along with healthy diet and exercise.
Generally, there are treatments to control symptoms or complications, help slow the growth of cysts, and help prevent or slow the loss of kidney function. Those include medication and lowering blood pressure, along with healthy diet and exercise.
But for those like CJ with the rare recessive or infantile disease, ARPKD – only about 10% of total PKD cases – there are few options. One-third need dialysis or transplant by age 10. Even with a new kidney, CJ likely will need another one in 10 to 20 years.
Still, said Dr. Sharma, the UT Health San Antonio nephrology division chief, there are takeaways from CJ’s case that instruct how patients in his condition could be managed, such as when kidney removal, or nephrectomy, should be planned. “And the fast-growing remaining kidney after the first nephrectomy is a phenomenon that could be examined in pre-clinical studies and may be helpful to future patients,” he said.
Also instructional was the parents’ painstaking decision-making throughout, which he calls “remarkable.” As for the couple, the takeaways were many.
A new perspective
“I think we’re all just one incident away from our lives being fundamentally changed in very profound ways,” dad said. “And nothing is ever guaranteed with anything, ever.
“We never anticipated having a kid with medical problems,” he said. “Nobody ever anticipates that. CJ has kind of taught me to treat every day like a good day, because CJ is healthy.”
And the lessons carry over to their professional lives.
“People sometimes assume that because I’m a kidney doctor that I had any familiarity with this disease,” mom said, noting that even pediatric kidney doctors see it uncommonly. “If you’re a pediatrician, they say kids are not little adults, and that’s very true. The same things don’t always apply.
“So, it definitely gave me a perspective of what was important,” she said. “It was a completely new world for me, and I had to learn so much. And fortunately, we had some great teams.”
 She said the whole experience has injected a more personal element to treating her patients. Asking more questions about their families, what their lives are like and how disease or treatment fits into their lives. And she can now speak to them as someone who not only has received a special gift, in CJ, but as someone who has given.
She said the whole experience has injected a more personal element to treating her patients. Asking more questions about their families, what their lives are like and how disease or treatment fits into their lives. And she can now speak to them as someone who not only has received a special gift, in CJ, but as someone who has given.
“The idea of looking for a living donor is not talked about a lot,” she said. “People are very scared to approach that conversation, to even ask or talk to family. I don’t think I’ve pushed for that in the past, or given my patients tools for how to start that conversation.
“Being on this side of it now,” she said, “I can tell them firsthand: It’s such an amazing thing that you can do.”
The University of Texas Health Science Center at San Antonio, also referred to as UT Health San Antonio, is one of the country’s leading health sciences universities and is designated as a Hispanic-Serving Institution by the U.S. Department of Education. With missions of teaching, research, patient care and community engagement, its schools of medicine, nursing, dentistry, health professions and graduate biomedical sciences have graduated 39,700 alumni who are leading change, advancing their fields, and renewing hope for patients and their families throughout South Texas and the world. To learn about the many ways “We make lives better®,” visit http://www.uthscsa.edu. Stay connected with The University of Texas Health Science Center at San Antonio on Facebook, Twitter, LinkedIn, Instagram and YouTube.
To see how we are battling COVID-19, read inspiring stories on Impact.



