Contact: Will Sansom, 210-567-2579, sansom@uthscsa.edu
SAN ANTONIO (Oct. 19, 2021) — Cancer that spreads, or metastasizes, to another area of the body is not typically as treatable as the primary tumor from which it originated. Survival from metastatic disease is generally poor.
What if a daily or weekly blood sample could monitor each patient’s risk of metastasis, indicating the need for aggressive therapy before cancer spread is established? That’s the ultimate goal of studies published by researchers from The University of Texas Health Science Center at San Antonio.
Sticky seeds
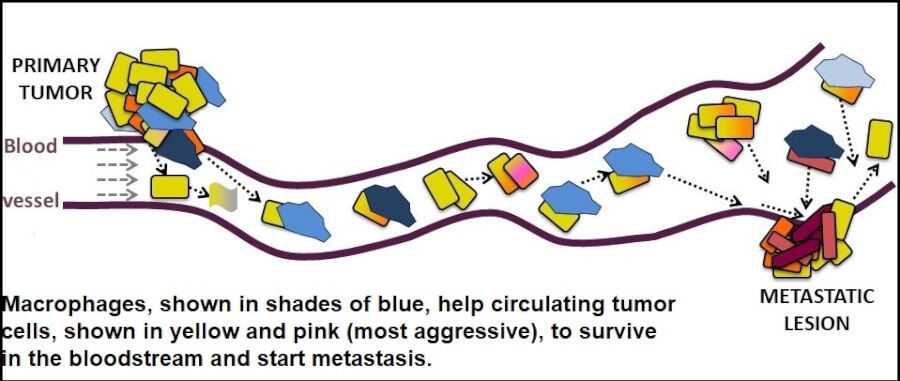
In the journal Cancer Research, authors including Maria E. Gaczynska, PhD, and Pawel Osmulski, PhD, report that blood-borne seeds of cancer, called circulating tumor cells (CTCs), have specific properties that can be measured. For example, CTCs are sticky and glom onto other cells called macrophages while hurtling through the bloodstream.

Cancer enablers
Macrophages are infection-fighting cells that can be either pro- or anti-inflammatory. It turns out that both kinds can act as accomplices to cancer spread.
“What is completely new, what we found here, is that both pro- and anti-inflammatory macrophages can be bad for the patient,” Dr. Gaczynska said. “Both can help circulating tumor cells to survive.”
Both types of macrophage can extend the microenvironment of a tumor to the bloodstream — to CTCs, Dr. Osmulski said.
Evidence that foretells risk
The study, conducted in human prostate cells provided by the Mays Cancer Center, home to UT Health San Antonio MD Anderson Cancer Center, indicated that the presence of macrophages, along with properties such as stickiness, can be an accurate biomarker of risk for metastasis.
“Actually, this is like a crystal ball,” Dr. Gaczynska said. “When we are looking at the nanomechanical properties, and when we are asking how many macrophages there are, we can tell if this patient is at risk of metastasis very soon.”
Current studies utilize an atomic force microscope at UT Health Science Center San Antonio, but the researchers seek to simplify the process to make it a bedside diagnostic. “We have an idea of how to do it,” Dr. Osmulski said.
Drug target
The finding about macrophages’ role in cancer is a key building block discovery.
“Because the majority of cancer patients die of metastasis, this is of very high medical relevance,” Dr. Osmulski said. “The interactions between CTCs and macrophages can be the target of anti-metastasis drugs.”
Cancer Research selected the study to be on the cover of the August issue of the journal.
Dr. Gaczynska and Dr. Osmulski are faculty in the department of molecular medicine of the health science center’s Joe R. and Teresa Lozano Long School of Medicine and are research investigators with the Mays Cancer Center.
Contacts with Macrophages Promote an Aggressive Nanomechanical Phenotype of Circulating Tumor Cells in Prostate Cancer
Pawel A. Osmulski, Alessandra Cunsolo, Meizhen Chen, Yusheng Qian, Chun-Lin Lin, Chia-Nung Hung, Devalingam Mahalingam, Nameer B. Kirma, Chun-Liang Chen, Josephine A. Taverna, Michael A. Liss, Ian M. Thompson, Tim H.-M. Huang and Maria E. Gaczynska
First published: May 27, 2021; cover article published August 2021, Cancer Research
http://doi.org/10.1158/0008-5472.CAN-20-3595
The University of Texas Health Science Center at San Antonio, also referred to as UT Health San Antonio, is one of the country’s leading health sciences universities and is designated as a Hispanic-Serving Institution by the U.S. Department of Education. With missions of teaching, research, patient care and community engagement, its schools of medicine, nursing, dentistry, health professions and graduate biomedical sciences have graduated 39,700 alumni who are leading change, advancing their fields, and renewing hope for patients and their families throughout South Texas and the world. To learn about the many ways “We make lives better®,” visit www.uthscsa.edu.
Stay connected with UT Health San Antonio on Facebook, Twitter, LinkedIn, Instagram and YouTube.
To see how we are battling COVID-19, read inspiring stories on Impact.



