Contact: Will Sansom, (210) 567-2579, sansom@uthscsa.edu
SAN ANTONIO (Sept. 22, 2022) — Debra Gutierrez of Von Ormy, Texas, near San Antonio has been an active person all her life. An ophthalmology technician at The University of Texas Health Science Center at San Antonio (UT Health San Antonio), she works in a clinic that sees scores of patients daily. But things changed for her in the summer of 2020, the early days of the pandemic before COVID-19 vaccines were available.
“My diagnosis with COVID was July 3, 2020,” Gutierrez, 49, said. “The main problem I had was massive migraines along with loss of smell, dizzy spells, body aches and blurry vision in my right eye.”
Although she never required hospitalization and was back at work after a month, her recovery was just beginning. In fact, she still doesn’t feel like she did prior to infection.
“I have episodes of disorientation, of not knowing where I am, including when I’m driving,” she said. “The longest episode was about 15 minutes. I had to grab my phone to give me directions home, because I had no idea where I was.”
Gutierrez keeps a diary of her symptoms and in May 2022 noticed that she started to stutter. “I never stuttered before,” she said.
The fog in her thinking is persistent, unending. “I tend to blank out even when I’m at work, and I’ve been doing this type of job for 26 years. I forget what I’m doing,” she said.

Gabriel de Erausquin, MD, PhD, professor of neurology in the Joe R. and Teresa Lozano Long School of Medicine at UT Health San Antonio, sees Gutierrez in his clinic. He prescribed medication to calm her when episodes occur.
De Erausquin is with UT Health San Antonio’s Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases, where one of the projects he leads is the Alzheimer’s Association Consortium on Chronic Neuropsychiatric Sequelae of SARS-CoV-2 infection. This is an initiative of research and clinical teams from around the world. Scientific leaders, including the Alzheimer’s Association and representatives from more than 25 countries, are working together with technical guidance from the World Health Organization to track the long-term impact of SARS-CoV-2 (also known as novel coronavirus, COVID-19) on the brain.
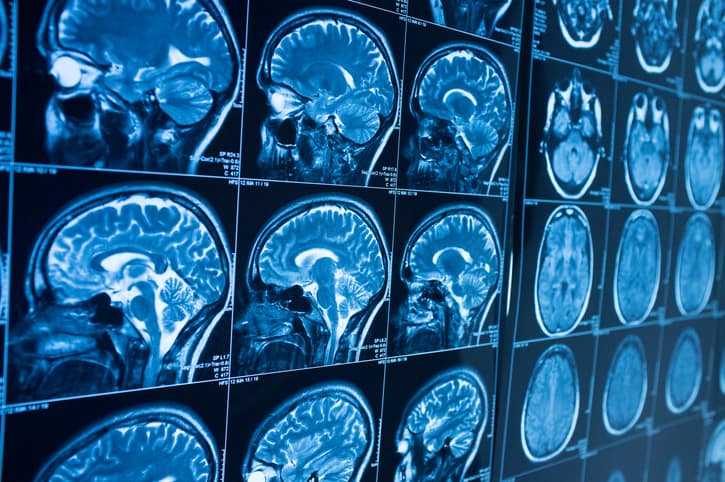
Debra Gutierrez is among the South Texas participants who will be evaluated at UT Health San Antonio upon entering the study and at specific points in time. Neuropsychological tests that assess aspects of learning and memory will be administered, and study volunteers will undergo brain imaging on the world’s most powerful MRI systems.
“No available evidence supports the notion that cognitive impairment after SARS-CoV-2 infection is a form of dementia, whether it is Alzheimer’s disease or related dementias or some other cause,” Dr. de Erausquin said. “The Alzheimer’s Association Consortium multinational initiative will provide data to answer this question as clearly as possible in a globally diverse set of participants.”
Persistent loss of smell is associated with brain changes. The olfactory bulb, which contains the brain cells that react to smell, is primarily where the COVID-19 virus enters the nervous system, Dr. de Erausquin said. Building on this information, the consortium aims to understand the effects that SARS-CoV-2 triggers in the brain.
In a peer-reviewed paper published Sept. 22 in Alzheimer’s & Dementia: Translational Research & Clinical Interventions, the consortium authors note, “It behooves the scientific and medical community to attempt to understand the molecular and/or systemic factors linking COVID-19 to neurologic illness, both short and long term.”
The article provides the roadmap for how those who wish to use the methodology developed by this large global research community will achieve this ambitious undertaking across multiple continents, languages and cultures.
Harmonization strategies and flexible study designs offer the possibility to include large samples of under‐represented racial and ethnic groups, Dr. de Erausquin said. Sharing of information, data and knowledge will enable future studies to have data generated from these diverse groups for years to come.
Debra Gutierrez, who still works full time, has a supportive husband, six adult sons and stepsons, and six grandchildren. Her experience, and the experiences of thousands around the world, will paint a fuller picture of what is happening in the brain post-COVID. Understanding how to address the cognitive issues caused by viral infections could lead to improved outcomes in the future.
“I was running marathons before, and I was working outside several days a week,” Gutierrez said. “I have lots of hope because I was a very active person.”
Funding for the consortium is provided in part by the Alzheimer’s Association.
The University of Texas Health Science Center at San Antonio (UT Health San Antonio), a primary driver for San Antonio’s $42.4 billion health care and biosciences sector, is the largest research university in South Texas with an annual research portfolio of $350 million. Driving substantial economic impact with its five professional schools, a diverse workforce of more than 7,000, an annual operating budget of more than $1 billion and a clinical practice that provides more than 2 million patient visits each year, UT Health San Antonio plans to add more than 1,500 higher-wage jobs over the next five years to serve San Antonio, Bexar County and South Texas. To learn about the many ways “We make lives better®,” visit http://uthscsa.edu.
Stay connected with The University of Texas Health Science Center at San Antonio on Facebook, Twitter, LinkedIn, Instagram and YouTube.