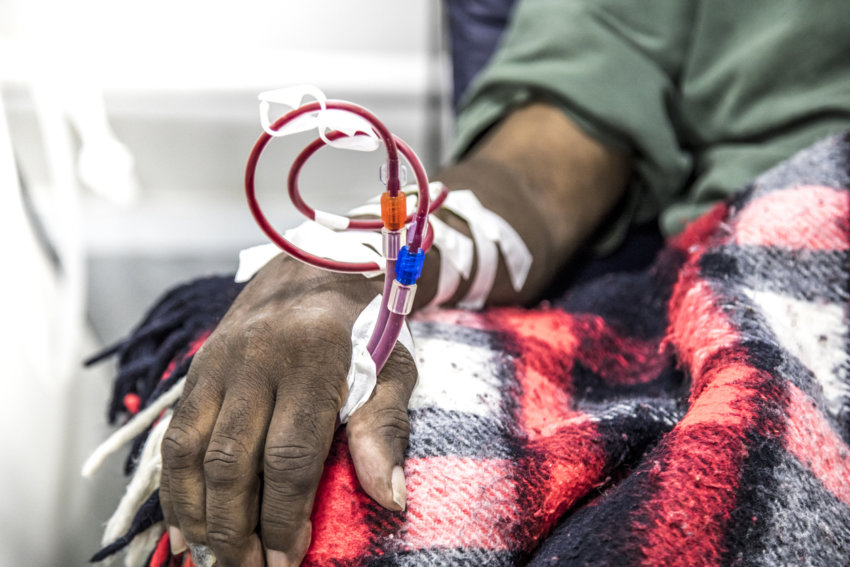
Some patients can wait for their treatment to be rescheduled if powerful storms or other extenuating circumstances intervene. This is not the case for dialysis patients.
“Dialysis patients are quite unique and many cannot wait, even for a few days,” said Kumar Sharma, MD, chief of nephrology at UT Health San Antonio. “They have to get dialyzed on a regular basis because their kidneys aren’t working, and if that doesn’t happen there is really no other course for them. Our patients are really connected to a lifeline, and that lifeline of dialysis requires a very big coordinated team effort that has to function at a high level at all times.”
The process requires dialysis machines, which need access to purified water and electricity, a dialysis technician, a dialysis nurse, a physician to provide orders for dialysis and assess patient status, and an administrator to conduct the process, said Dr. Sharma, who was the attending physician for the nephrology consult service during the week-long storm.
The storms hampered access to purified water and affected water pressure and electricity. Many providers were unable to get to work. Despite those challenges, the combined nephrology teams of University Health and UT Health San Antonio were able to find a way to marshal the resources necessary to dialyze hundreds of patients at University Hospital, both inpatient and outpatient —including between 60 and 70 inpatients daily, up from the typical 20 to 30. The coordination of outpatient treatment was a similarly impressive accomplishment, Dr. Sharma said.
“This was really a profound event which was essentially a disaster response and truly life-saving of hundreds of lives,” he said.
Some areas hospitals were not able to perform dialysis during the storm, which increased the need for care at University Hospital.
“Some of our patients that were admitted to University Hospital were able to be dialyzed at the VA and reduce the load at the hospital,” a workaround made possible because approval from the state was obtained rapidly — within 24 hours, Dr. Sharma said.
“We were able to coordinate all of those processes in a matter of 24 hours to identify how these patients could be dialyzing in the hospital setting and having the staff come and work 24/7 for three or four days,” he said. “The logistics had to be taken care of on an instant notice. There were many heroic stories.”
Among them, he said, were the University Health nurses who threw themselves into long hours of caring for patients and “slept in the hospital overnight wherever they could find space and literally risked their lives coming into work on icy roads.”
Other feats included dialysis technicians working to get purified water ready; nephrology fellows — some not even in service at the hospital — showing up to triage patients, write orders and see patients in the emergency room; and inpatient nephrology fellows finding a way to report to work despite a lack of power in their own homes or needing to make care plans for their young children at home; and the Herculean efforts by those coordinating the effort.
“The team work was truly phenomenal,” Dr. Sharma said.