Novel AI algorithm precisely quantifies perivascular spaces that signal risk of stroke.
Contact: Will Sansom, 210-567-2579, sansom@uthscsa.edu
SAN ANTONIO (July 13, 2023) — An artificial intelligence (AI) tool developed at The University of Texas Health Science Center at San Antonio accurately counts brain lesions on MRI scans within seconds. Once it is adapted to the clinic, the AI tool should help neuroradiologists to evaluate patients’ brain diseases at earlier stages.

“Certain kinds of brain lesions are tremendously difficult to quantify without AI,” said researcher Mohamad Habes, PhD, of the health science center’s Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases. Habes is assistant professor of radiology and director of the Biggs Institute neuroimaging core.
In a study published April 24 in JAMA Network Open, Habes and colleagues from eight institutions demonstrated the AI tool’s utility in identifying and counting enlarged perivascular spaces (ePVS’s). These spaces, filled with cerebrospinal fluid, surround arteries and veins and are a marker of cerebral small-vessel disease that can lead to stroke and dementia. The study was a follow-up analysis of 1,026 individuals who participated in the Multi-Ethnic Study of Atherosclerosis (MESA).
“We have developed an innovative deep-learning tool to precisely quantify every single enlarged perivascular space in the brain and provide us with a map of the patient’s small-vessel disease,” Habes said.
Taking a painstaking task and making it possible
Before this tool, ePVS’s were ignored because of the difficulty of counting them on MRI scans.
“On average a middle-aged person might have maybe 500 or 600 of these small spaces on an MRI,” Habes said. “Think about a neuroradiologist who is going to sit down and count all of them. That’s not really going to happen. He or she would spend one or two hours per scan, or even more, and that amount of laborious effort is not feasible in the workflow of a busy clinic.”
The team described the automated deep-learning method for ePVS detection in the journal Neuroimage: Reports on March 7. “We have trained an algorithm with expert knowledge to be able to quantify these lesions on its own,” Habes said. “This tool recognizes them, tells us their exact locations, counts them and tells us their volumes. It tells us a ton of information about them, far more than what a human can do.”
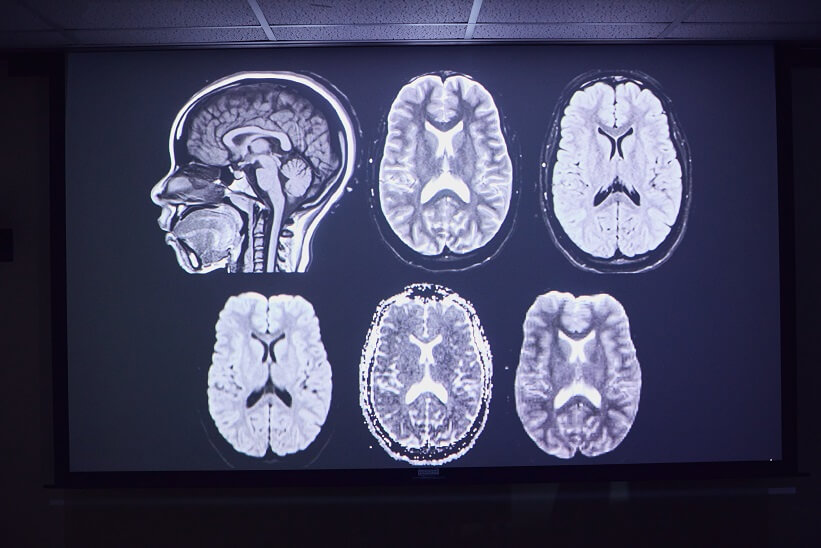
In the JAMA Network Open report, Habes and coauthors studied enlarged perivascular spaces throughout the brain.
“Before, people were not able to do whole-brain ePVS quantification,” Habes said. “We can now do it with our advanced deep learning tools. In our study, we realized that enlarged perivascular spaces in two regions, the basal ganglia and the thalamus, are the most significant lesions because they showed association with stroke and small-vessel disease markers.”
The basal ganglia is a deep-brain region important for neurodegenerative disorders and is related to movement and decision-making, Habes said. The thalamus, a region near the basal ganglia, is related to sensory functions such as taste and touch.
The researchers’ hope is that the AI tool for enumerating brain lesions will be further studied at the Alzheimer’s Disease Research Centers (ADRCs), which are U.S. National Institute on Aging-Designated Centers of Excellence. The South Texas ADRC, the only such center in Texas, is a collaboration of UT Health Science Center San Antonio’s Biggs Institute with The University of Texas Rio Grande Valley.
 “This is a great breakthrough for our ADRC, which is focusing a lot on cerebrovascular disease and its contribution to dementia,” Habes said. “This is one of the unique themes of our ADRC, and we think our novel AI methodology can benefit large-scale studies conducted across the nation’s ADRCs.”
“This is a great breakthrough for our ADRC, which is focusing a lot on cerebrovascular disease and its contribution to dementia,” Habes said. “This is one of the unique themes of our ADRC, and we think our novel AI methodology can benefit large-scale studies conducted across the nation’s ADRCs.”
The AI tool leverages the power of UT Health Science Center San Antonio’s Genie supercomputer, Habes said.
Assessment of Risk Factors and Clinical Importance of Enlarged Perivascular Spaces by Whole-Brain Investigation in the Multi-Ethnic Study of Atherosclerosis
Sokratis Charisis, MD; Tanweer Rashid, PhD; Hangfan Liu, PhD; Jeffrey B. Ware, MD; Paul N. Jensen, PhD; Thomas R. Austin, PhD; Karl Li, MD, PhD; Elyas Fadaee, MD; Saima Hilal, MD, PhD; Christopher Chen, MD; Timothy M. Hughes, PhD; Jose Rafael Romero, MD; Jon B. Toledo, MD, PhD; Will T. Longstreth Jr, MD; Timothy J. Hohman, PhD; Ilya Nasrallah, MD, PhD; R. Nick Bryan, MD, PhD; Lenore J. Launer, PhD; Christos Davatzikos, PhD; Sudha Seshadri, MD; Susan R. Heckbert, MD, PhD; Mohamad Habes, PhD
First published: JAMA Network Open, April 24, 2023
https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2803993
The University of Texas Health Science Center at San Antonio (UT Health San Antonio), a primary driver for San Antonio’s $44.1 billion health care and biosciences sector, is the largest academic research institution in South Texas with an annual research portfolio of more than $360 million. Driving substantial economic impact with its six professional schools, a diverse workforce of 7,900, an annual operating budget of $1.23 billion and clinical practices that provide 2.6 million patient visits each year, UT Health San Antonio plans to add more than 1,500 higher-wage jobs over the next five years to serve San Antonio, Bexar County and South Texas. To learn about the many ways “We make lives better®,” visit UTHealthSA.org.
The Glenn Biggs Institute for Alzheimer’s and Neurodegenerative Diseases is dedicated to providing comprehensive dementia care while advancing treatment through clinical trials and research. The Biggs Institute is a National Institute on Aging (NIA)-designated Alzheimer’s Disease Research Center (ADRC). In addition to patient care and research, the Biggs Institute partners with the School of Nursing at UT Health San Antonio to offer the Caring for the Caregiver program.
Stay connected with The University of Texas Health Science Center at San Antonio on Facebook, Twitter, LinkedIn, Instagram and YouTube.