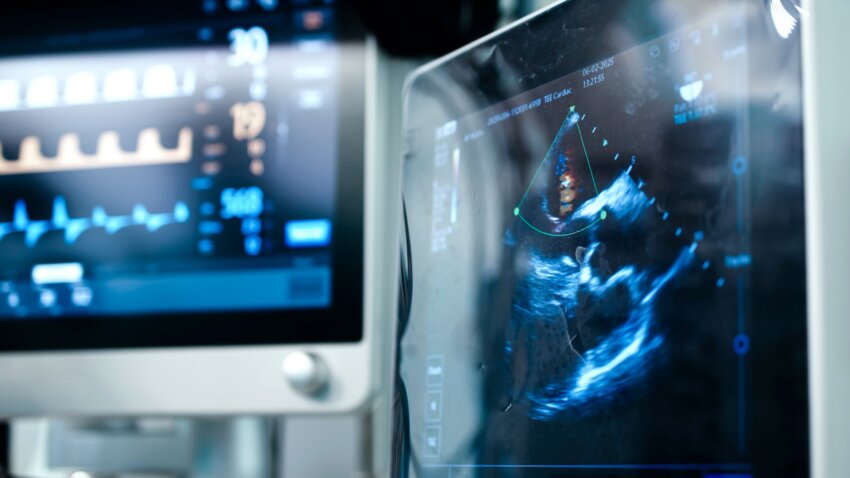
By bringing imaging directly to the bedside, point-of-care ultrasound, or POCUS, allows providers to make faster, more informed decisions in real time. As POCUS use continues to expand, The Joe R. and Teresa Lozano Long School of Medicine at The University of Texas at San Antonio (UT San Antonio) is at the forefront of a growing effort to ensure clinicians are trained to use it effectively.
Essential technology

Because of its portability and safety, POCUS devices have become essential to how clinicians diagnose and treat patients, so much so that many medical professionals refer to it as the “stethoscope of the 21st century,” said Nilam Soni, MD, SFHM, FACP, professor of medicine and director of Critical Care Ultrasound Education at the Long School of Medicine, and director of the VA Point-of-Care Ultrasound Training Program for the Department of Veteran Affairs.
Soni explained that POCUS is often the go-to bedside tool for evaluating patients because the devices are small and portable, making it a much quicker diagnostic imaging option, and because it allows clinical decision-making at the bedside with the patient.
“Ultrasound doesn’t expose patients to radiation,” Soni said. “For patients who need frequent imaging, they can be exposed to hundreds or even thousands of times more cumulative radiation with CT scans compared to ultrasound. So, ultrasound is a much safer, preferred modality in patients with chronic illnesses, especially young patients.”
POCUS is also a more available technology worldwide, including resource-limited and rural settings in the United States. Globally, many hospitals lack the infrastructure and staff required to operate large imaging machines, making ultrasound a critical tool.
Meeting a growing need for training
As the use of POCUS expands, so does the need to train clinicians across all levels of care.
While many medical schools now offer ultrasound training across specialties, a gap remains for practicing clinicians who did not learn how to use POCUS during their formal education.
“It’s a bit of a catch-22,” Soni said. “Clinicians can have a hard time getting equipment if they’re not trained, but without equipment, they can’t practice and get trained!”
Addressing the training gap has become a central focus for Soni and his team at the Long School of Medicine.
 A global leader in POCUS education
A global leader in POCUS education
Over the past decade, the Long School of Medicine has emerged as a global leader in POCUS training.
“We’ve been leading this not only for San Antonio or Texas, but for the country, and really for the world,” he said.
A cornerstone of that effort is the university’s annual continuing medical education (CME) course. Since launching in 2013 with about two dozen participants, the program has grown into one of the largest institutional POCUS training events in the country.
“We started with about 18 to 24 participants, and it filled up,” Soni said. “Now it’s grown into multiple courses, with more than 250 people on site.” Participants have come from nearly all 50 states and even other countries.
The program now includes dedicated tracks in adult, pediatric/neonatology, and advanced cardiac ultrasound. All sessions have been reaching capacity and maintaining waiting lists.
Writing the book on ultrasound
Beyond offering the POCUS CME course, Soni and his colleagues also authored a widely used POCUS textbook that has been translated into multiple languages and distributed globally. The first edition earned recognition from the British Medical Association, and a third edition is now in development.
“When people open the book and see it comes from UT Health San Antonio, the academic health center of UT San Antonio, it really stands out,” Soni said.
 Hands-on learning at scale
Hands-on learning at scale
A defining feature of the POCUS CME course is its emphasis on hands-on training.
The curriculum focuses on four core components: basic knowledge, image acquisition, image interpretation and clinical integration.
The course brings together expert faculty from across the country and provides small-group scanning sessions, allowing learners to gain real-world experience.
“Even though it’s a large course, we try to individualize the experience,” he said. “If someone wants to focus on specific skills, we pair them with the right faculty.”
Improving care at the bedside
The impact of POCUS training is felt directly in patient care.
“The bottom line is that better training equates to improved diagnostic accuracy,” Soni said.
With ultrasound at the bedside, clinicians can more quickly narrow diagnoses, reducing the need for multiple tests and minimizing delays.
“Instead of ordering a battery of tests, you can focus your workup and care based on what you see,” he said.
POCUS also improves procedural safety by allowing clinicians to visualize procedures like inserting a needle in real time.
“If we know where the needle tip is going, we have fewer complications,” Soni said. “That’s become the standard of care.”
As technology advances, including the integration of artificial intelligence, POCUS is expected to expand even further, improving access to care in both urban and rural settings.
With its growing programs and global reach, the Long School of Medicine at UT San Antonio continues to shape the future of ultrasound-guided medicine by training clinicians to deliver faster, safer and more precise care.